Prevalent Cancer type
Et al for diagnoses is made up of a heterogenous group of diagnoses where there has only been one patient with that diagnosis
Sheffield Children’s NHS Foundation Trust is one of only three dedicated children’s hospital trusts in the UK and provides integrated healthcare for children and young people, including community and mental health care as well as acute and specialist services
Sheffield Children’s aim is to provide a healthier future for children and young people by making physical activity an integral part of their treatment plans, whilst also offering more resources to support staff, patients and their families
Chosen Pathway
One of the three pathways Sheffield Children’s chose to implement as part of the Moving Healthcare Professional’s Active Hospital workstream was Paediatric Oncology. Childhood cancer survivors have an increased risk of long-term health conditions with excess morbidity and mortality in adulthood. Research demonstrates improved outcomes with increased physical activity. Inpatients often require bespoke physical activity advice based upon their clinical condition, care and mobility.
Referral to an assessment by EPAT and development of personalised programme
Active options for patients required to be in isolation
Active play on ward
Movement on ward encouraged
Encouraged to leave the ward and walk round hospital / adjacent park if clinically appropriate
Moving Medicine “More minutes“ conversations
Physical Activity Plan
EPAT OP sessions (alongside ongoing cancer treatment)
Invitation to annual Do it for You activity day
PA plan in community
Liaison with community providers (eg schools)
Referral to a community based EPAT for links in to school and community based activities
Staff Training
Physical Activity Clinical Champions training
Active Conversation training
Governance
Report back to Senior Management Team
Environmental
Completed Planned refurbishment of ward to encourage movement.
Interactive technology in playroom to encourage movement
Provision for remaining active in transplant isolation rooms
Co-located ward and clinic space enabling easy access to gym equipment
Communications/Promotion
Internal
AH promoted to staff on the intranet and in team meetings
External
Press releases
Presentations at conferences and national meetings
Intervention overview
A FASED approach was used to guide the set up and continual development of this intervention.
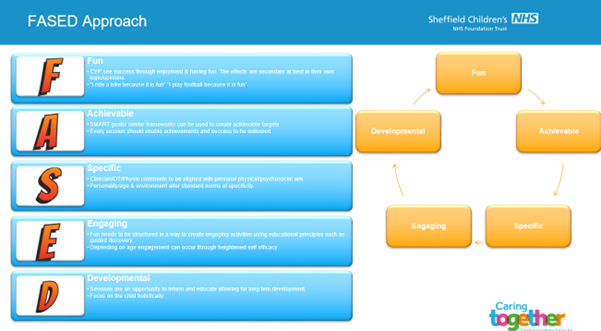
Key components include:
– A dedicated Children’s Exercise and Physical Activity Therapist (CEPAT) was appointed as part of the pilot to lead on working with, and supporting, children and families throughout their treatment and beyond with a focus on the benefits of physical activity (PA) and how to achieve appropriate levels for each patient
-Ward staff educated on the benefits of physical activity through PACC and Active Conversations training and a peer support group
– Tools, resources and activities were embedded into the environment including the use of a PA calculator on admission, printed resources for patients and staff, i-CAN tool above beds, a PA passport, PE lessons for inpatients, 1:1 sessions of exercise therapy
-Ongoing support for patients provided via a PA discharge plan including referrals to local service and handover information to schools
-Data was collected for internal audit to support ongoing improvements to the intervention as well as to contribute to the independent evaluation carried out as part of the Moving Healthcare Professionals Programme (MHPP)
The Physical Activity calculator was used to calculate activity levels at the initial assessment
Guides to support HCP have conversations with their patients about PA. Specific to around 20 conditions, for adults and for children and tailored the amount of time available in a consultation. Also provide a selection of resources/support and activities for patients.
There is a :
As a result of the ward refurbishment there is now a bigger footprint. There is a new playroom that has interactive technology incorporated in to its design. Children are encouraged to move around the room interacting with images on the floor and walls. Children are encouraged to move around the ward through play (scooters and cars are provided). Non isolation rooms are at the opposite end of the ward to the schoolroom and playroom which means that patients have to walk to the other end of the ward to access these. Although discussions were held about designing ward décor to encourage activity this has not been fully realised and work is ongoing.
The I CAN is a patient centred enablement tool that was developed by Moving Medicine to help staff identify functional level of patient quickly and easily. This allows staff to facilitate the appropriate level of functional assistance required for each patient to support their independence as far as possible.
It is designed to be displayed at the end of the bed, and our I CANs were laminated to comply with infection control policy.
Physical Activity Clinical Champions training was given to all staff within this pathway. This is peer to peer face to face or online interactive training delivered by a healthcare professional. It is designed to increase knowledge, skills and confidence in healthcare professionals around the benefits of physical activity to improve the quantity and quality of conversation with patients.
Active Conversations is a practical, evidence-based online learning course developed by clinicians, for clinicians that teaches how to have quick, effective and positive conversations that encourage patients to do more physical activity.
Material was produced by to support the internal/external promotion of the Active Hospitals work. This included:
-Posters
-Presentations at conferences
-Published info (Saskia etc) on the intranet
-Local newspapers etc
In this section you will find some of the outcomes from the pathway.
Oncology overview up to Jan 2023
Brief numbers:
84 patients have been referred to the exercise and physical activity programme. Of the 84 patients who have been referred 29 have complete pre and post testing. A further 10 have completed the initial testing and have either not completed the post intervention testing or have not finished the intervention at this point. 46 patients opted to receive face to face or virtual one to one sessions with a further 17 opting to have access to support such as online programs or referrals/support to other opportunities. 21 patients either declined to receive any support or declined to correspond.
Results for intervention:
| Metric | PACES | Sit To Stand | Standing March |
| Change | -2.1 | 9 | 18 |
Average PACES (physical activity enjoyment scale) score has decreased on average by 2.1 points, this suggests a small beneficial change in attitudes towards physical activity as the lower the recorded score the better the outcome. 2-minute sit to stand and 2-minute standing march tests have increased by 9 & 18 repetitions respectively suggesting a positive impact on physical function.
I think it definitely exceeded my expectations, both for myself and for what I thought the programme was going to be. I didn’t think I would get to this good a point. I’ve got so much more independence back now, from being in a wheelchair to now is such a massive difference.